 In 1989, Andrew Livingstone was born without a blemish, but two weeks later, a strawberry red growth began to bloom on his upper lip. At age three months, the mass enlarged quickly, extending up to his nose. It became an open sore, which would scab over, only to ulcerate again and again. Andrew’s pediatrician diagnosed the condition as a hemangioma and referred his parents, Seth and Marcy, to renowned expert, plastic surgeon John Mulliken, MD, at Children’s Hospital Boston.
In 1989, Andrew Livingstone was born without a blemish, but two weeks later, a strawberry red growth began to bloom on his upper lip. At age three months, the mass enlarged quickly, extending up to his nose. It became an open sore, which would scab over, only to ulcerate again and again. Andrew’s pediatrician diagnosed the condition as a hemangioma and referred his parents, Seth and Marcy, to renowned expert, plastic surgeon John Mulliken, MD, at Children’s Hospital Boston.
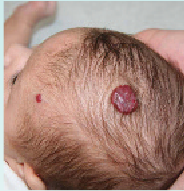
A hemangioma is a tangled mass of poorly formed blood vessels typically found on the head or neck. This noncancerous growth is the most common tumor of infancy and childhood. “Most of these vascular tumors are in the skin, but they can occur in any organ, including the liver and even the iris of the eye,” says Dr. Mulliken, co-director of Children’sVascular Anomalies Center, the first inter – disciplinary center of its kind in the country. “About 20 percent of affected children have multiple hemangiomas.” Hemangiomas typically develop during early infancy, initially appearing as a pale red stain, bruise, or cluster of spidery blood vessels. During the first year of life, they grow rapidly into a firm mound, and then over the next five years or so, shrink and fade away slowly in a process known as “involution.” Some hemangiomas are present at birth at a nascent or early stage of development. Although hemangiomas sometimes run in families, they are not strictly hereditary. Fair-skinned babies develop hemangiomas more often than babies with darker complexions. And girls are affected 3 to 5 times as often as boys. Hemangiomas are also more common in premature babies with low birth weight as well as in multiple births.
What causes hemangiomas? Using samples of infantile hemangioma provided by Dr. Mulliken, Joyce Bischoff, PhD, and her colleagues in Children’s Vascular Biology Program have shown that the answer is an abnormality in a primitive stem cell that divides and develops into specialized tissues, including blood vessels.
When and How to Treat
In 9 out of 10 cases, diagnosis of a vascular tumor can be made based on patient history and a physical examination. But magnetic resonance imaging (MRI) and ultrasonography may also be needed to confirm the diagnosis or determine the extent of a large lesion in the airway or brain. While many hemangiomas disappear without lasting effects, some require treatment. “Surgical resection is indicated when a hemangioma obstructs breathing or vision, or is ulcerated, bleeding, or deforming facial features,” says Dr. Mulliken. “Drug therapy is often required for large hemangiomas in the liver, which can cause congestive heart failure, and even hypothyroidism. “While deep lesions regress to relatively normal skin,” adds Dr. Mulliken, “superficial lesions can result in tiny red capillaries, sagging, thin skin, fibrofatty tissue, and scarring—particularly if ulceration has occurred. Even small hemangiomas stretch the skin and may leave behind a bulging, fatty lump that requires treatment.” Dr. Mulliken recommends that all infants or children with problematic hemangiomas be seen at a vascular anomaly center at a major teaching hospital. At Children’s Hospital Boston, an interdisciplinary team, composed of surgeons, dermatologists, interventional radiologists, neuroradiologists, pathologists, nurse practitioners, and other specialists, meets weekly to discuss treatment plans for patients with hemangiomas and other vascular anomalies. The most common medical treatment for infant hemangiomas involves daily oral corticosteroid, decreasing over a 10-month period. However, during the past two years, some doctors have begun using an alternative for shrinking lesions—a beta- blocker called propranolol. French doctors accidentally discovered this new therapy when using the drug to treat two infants with heart problems, who also happened to have hemangiomas. Some doctors believe propranolol, which has fewer side effects than steroids, should be the first-line treatment for this tumor. Surgical intervention may be needed for larger hemangiomas. “Operations may be undertaken during the proliferative, involuting—year 2 to 5 or so—and involuted stages,” says Dr. Mulliken. “But it is important to go to a surgeon who has experience handling hemangiomas at these different phases. Operating on something that’s downsizing is not like working on a sculpture of stone. Each hemangioma is unique–some can be trimmed in one operation, while others require a series of operations. “Laser treatment is not indicated during infancy,” he adds. “When the child is older and the lesion is involuted, it plays an important role and can be used to fade tiny residual capillaries.” Andrew Livingstone is now 20, and his hemangioma is a thing of the past. He is thriving as a third-year student at Cornell University, majoring in Industrial and Labor Relations.
Starting at age 4, he underwent several operations to remove excess skin left as the hemangioma receded. Later, he had laser treatments to fade remaining discoloration. “Dealing with his own physical imperfections has enabled Andrew to develop a sensitivity that does not come automatically,” says his father. “He’s very attuned to others. In high school, he was the student founder of the athlete-to-athlete club, which organized and paired special needs kids with varsity athletes. He sees people for what they are, not just skin-deep.”
